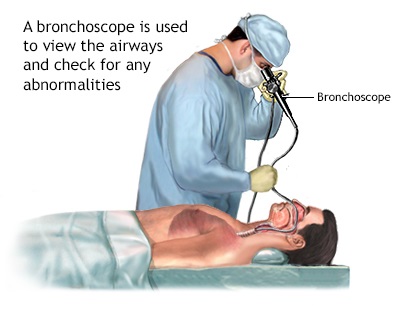
Branchoscopy
What is Bronchoscopy?
Bronchoscopy is a minimally invasive procedure that lets your doctor look inside your airways and lungs. It’s usually done with a flexible bronchoscope, a thin, bendable tube with a light and tiny camera at one end. In some cases (such as having a large object stuck in your airway), your provider may need to use a rigid bronchoscope.
Healthcare providers use bronchoscopy to find out what’s causing problems in the lungs, trachea (windpipe) or throat. They can also use the procedure to take tissue samples (biopsy) or insert a stent (a small tube) in the airway to keep it open.
When is Bronchoscopy Needed?
A healthcare provider may recommend bronchoscopy for many different reasons. Some of the most common are:
- Diagnosing lung disease or other causes of shortness of breath.
- Following up after an X-ray or CT scan showed possible signs of a tumor (cancer) or lung damage.
- Assessing and treating blockages in your airways.
- Evaluating lymph nodes (part of your immune system) near your lungs.
- Taking samples of mucus or tissue.
TEST DETAILS
How do I Prepare for Bronchoscopy?
Your healthcare providers will give you specific instructions about how to prepare.
You’ll need to fast (not eat or drink) for a certain period of time before the procedure. You may also have to stop taking certain medications that can thin your blood, like warfarin.
You will have a sedative or anesthesia before the procedure. You should plan on having someone available to drive you home afterward.
What happens during a Bronchoscopy?
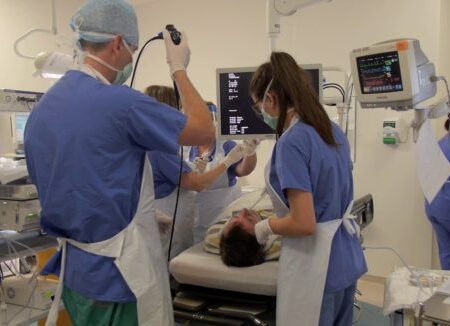
The entire bronchoscopy procedure typically takes from 30 minutes to a couple of hours. It’s usually performed in a hospital as an outpatient procedure. During a bronchoscopy:
- You lie on a bed or table with your head propped up.
- Your provider inserts an IV into your arm to deliver a sedative to help you relax. Some people may prefer to be asleep for the procedure. Rigid bronchoscopy and certain types of flexible bronchoscopy usually requires general anesthesia (being asleep). You and your provider can decide if general anesthesia is right for you.
- Your provider applies a numbing spray to your mouth (or nose) and throat.
- Once the area is numb and you are sedated, the provider inserts the bronchoscope through your nose or mouth and down into your windpipe to your lungs.
- After the procedure, the provider gently removes the bronchoscope. Your healthcare team monitors your condition until you are fully awake.
What happens after a Bronchoscopy?
Bronchoscopy is an outpatient procedure, so you will not need to spend the night in the hospital. Patients can typically go home within a few hours of the procedure.
Your healthcare team will monitor you after the procedure to ensure you are breathing and swallowing properly. It will take a couple of hours for the numbness in your throat to wear off. You may have a sore throat, cough or hoarseness after the procedure for the next 24 hours.
Your healthcare team will let you know when you should expect test results and when you should schedule a follow-up appointment.
What are the risks of a Bronchoscopy?
Bronchoscopy is a very safe procedure, but there is a slight risk of:
- Bleeding.
- Infection.
- Lung collapse.
RESULTS AND FOLLOW-UP
When should I know the results of the Bronchoscopy?
Ask your healthcare team when you can expect results. If they took biopsies during the procedure, the results should be available within a few days.
When should I call my Doctor?
Call your healthcare team if you have any of the following symptoms, which can indicate an infection, collapsed lung or other problem:
- Chest pain.
- Difficulty breathing.
- Persistent fever.
- Persistent cough or coughing up blood.
- Signs of pneumonia.
A Note from Dr. Agrawal
Bronchoscopy is a safe procedure that helps your healthcare provider diagnose the cause of lung and airway problems. In some cases, providers also use bronchoscopy to treat lung and airway conditions. This outpatient procedure involves inserting a flexible tube through your mouth or nose and down into your lungs. If your healthcare provider recommends bronchoscopy, you’ll get more details to prepare.
FAQs
What are the facilities available at the clinic?
The following facilities are available:
- Pulmonary function testing (Spirometry)
- Bronchoscopy
- EBUS
- Sleep studies (polysomnography)
- Thoracoscopy
- Lung cancer chemotherapy
I snore. Do I need to undergo a sleep study test?
It is not necessary that all persons who snore need to undergo a sleep study. There should be associated features to label it a disease. You should seek consultation from a sleep specialist in this case, who will screen you appropriately.
What will happen to my body if I sleep less?
Sleep is one of the key factors that determine the health of an individual. How one wakes up in the morning is a fair indicator whether one is getting a proper sleep or not. Therefore, if you have been snoozing your alarm too often, you might be damaging your own health. Experts believe that under normal circumstances, one should be able to wake up refreshed. And if you are not then you might be suffering from a sleep disorder. This can cause neurological changes in your body and can reduce the productivity at work. Moreover, in the short run it can cause memory problems and severe hormonal changes in your body.
Whatv is Pulmonary sleep test?
PFT measures how much air you can breathe in and out and how fast you can do it and how well your lungs are working to deliver oxygen to your blood. PFT is a painless test and a technician will ask you to take a deep breath and then blow as hard as you can into a tube connected to PFT machine.
PFT is the most important test for the diagnosis and management of COPD. PFT is similar to ECG of the lungs