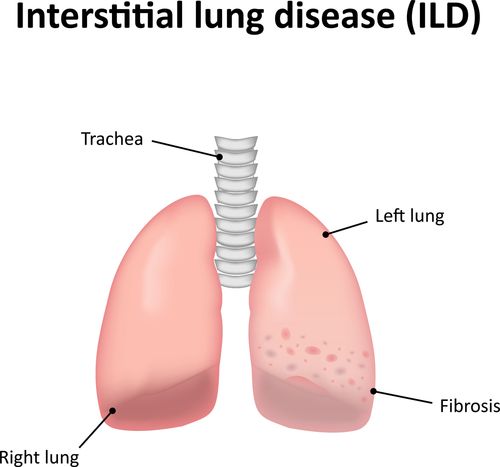
Interstitial lung disease (ILD)
Interstitial lung disease refers to a group of about 100 chronic lung disorders characterized by inflammation and scarring that make it hard for the lungs to get enough oxygen. The scarring is called pulmonary fibrosis.
The symptoms and course of these diseases may vary from person to person. The common link between the many forms of the disease is that they all begin with inflammation.
- Bronchiolitis: inflammation of the small airways (bronchioles).
- Alveolitis: inflammation of the air sacs where oxygen and carbon dioxide exchange in the blood takes place (alveoli).
- Vasculitis: inflammation that involves the small blood vessels (capillaries).
Fibrosis leads to permanent loss of your lung tissue’s ability to carry oxygen. The air sacs, as well as the lung tissue around the air sacs and the lung capillaries, are destroyed when the scar tissue forms.
The disease may run a gradual course or a rapid course. People who have it may notice variation in symptoms, from very mild to moderate to very severe. The condition may stay the same for a long time or it may change quickly. The course of the disease is unpredictable. If it progresses, the lung tissue thickens and becomes stiff, making breathing more difficult.
What causes interstitial lung diseases?
The cause of interstitial lung disease is not known. Major contributing factors include:
- Smoking
- Certain drugs or medicines
- Exposure to substances at work or in the environment such as organic or inorganic dusts
- Certain connective tissue or collagen diseases and sarcoidosis
- Family history
- Radiation treatment
What are the symptoms of interstitial lung diseases?
Each person may experience interstitial lung disease differently, but the most common symptoms include:
- Shortness of breath, especially with activity
- Dry, hacking cough that does not produce phlegm
- Extreme tiredness and weakness
- Loss of appetite
- Unexplained weight loss
- Discomfort in the chest
- Labored breathing, which may be fast and shallow
- Bleeding in the lungs
The symptoms of interstitial lung diseases may look like other lung conditions or medical problems. Talk with your healthcare provider for a diagnosis.
How are interstitial lungs diseases diagnosed?
In addition to a complete medical history and physical exam, the healthcare provider may also request pulmonary function tests. These tests help to measure the lungs’ ability to move air into and out of the lungs. They may include:
Spirometry
A spirometer is a device used to check lung function. Spirometry is one of the simplest, most common tests. It may be used to:
- Determine how well the lungs receive, hold, and move air
- Look for lung disease
- See how well treatment is working
- Determine the severity of a lung disease
- Find out whether the lung disease is restrictive (decreased airflow) or obstructive (disruption of airflow)
Peak flow monitoring
This device is used to measure the how fast you can blow air out of the lungs. Disease-related changes can cause the large airways in the lungs to slowly narrow. This will slow the speed of air leaving the lungs. This measurement is very important in evaluating how well or how poorly the disease is being controlled.
Chest X-rays
This test takes pictures of internal tissues, bones, and organs.
Blood tests
Arterial blood gas may be done to check the amount of carbon dioxide and oxygen in the blood. Other blood tests may be used to look for possible infections.
CT scan
This test uses a combination of X-rays and computer technology to produce horizontal, or axial, images (often called slices) of the body. CT scans are more detailed than regular X-rays.
Bronchoscopy
This is direct exam of the main airways of the lungs (bronchi) using a flexible tube called a bronchoscope. Bronchoscopy helps to evaluate and diagnose lung problems, check blockages, take out samples of tissue or fluid, and help remove a foreign body. Bronchoscopy may include a biopsy or bronchoalveolar lavage.
Bronchoalveolar lavage
Removing cells from the lower respiratory tract to help identify inflammation and exclude certain causes.
Lung biopsy
Removing a small piece of tissue from the lung so it can be examined under a microscope
FAQs
I snore. Do I need to undergo a sleep study test?
It is not necessary that all persons who snore need to undergo a sleep study. There should be associated features to label it a disease. You should seek consultation from a sleep specialist in this case, who will screen you appropriately.
What are the facilities available at the clinic?
The following facilities are available:
- Pulmonary function testing (Spirometry)
- Bronchoscopy
- EBUS
- Sleep studies (polysomnography)
- Thoracoscopy
- Lung cancer chemotherapy
What will happen to my body if I sleep less?
Sleep is one of the key factors that determine the health of an individual. How one wakes up in the morning is a fair indicator whether one is getting a proper sleep or not. Therefore, if you have been snoozing your alarm too often, you might be damaging your own health. Experts believe that under normal circumstances, one should be able to wake up refreshed. And if you are not then you might be suffering from a sleep disorder. This can cause neurological changes in your body and can reduce the productivity at work. Moreover, in the short run it can cause memory problems and severe hormonal changes in your body.
Whatv is Pulmonary sleep test?
PFT measures how much air you can breathe in and out and how fast you can do it and how well your lungs are working to deliver oxygen to your blood. PFT is a painless test and a technician will ask you to take a deep breath and then blow as hard as you can into a tube connected to PFT machine.
PFT is the most important test for the diagnosis and management of COPD. PFT is similar to ECG of the lungs