Endobronchial ultrasound (EBUS)
Endobronchial ultrasound (EBUS) is a minimally invasive but highly effective procedure used to diagnose lung cancer, infections, and other diseases causing enlarged lymph nodes in the chest. UC San Diego Health was one of the first centers on the West Coast to offer EBUS and remains a regional leader in volume and overall experience.
Why is EBUS used?
EBUS allows physicians to perform a technique known as transbronchial needle aspiration (TBNA) to obtain tissue or fluid samples from the lungs and surrounding lymph nodes without conventional surgery. The samples can be used for diagnosing and staging lung cancer, detecting infections, and identifying inflammatory diseases that affect the lungs, such as sarcoidosis or cancers like lymphoma.
What makes EBUS different?
 During a conventional diagnostic procedure, surgery known as mediastinoscopy is performed to provide access to the chest. A small incision is made in the neck just above the breastbone or next to the breastbone. Next, a thin scope, called a mediastinoscope, is inserted through the opening to provide access to the lungs and surrounding lymph nodes. Tissue or fluid is then collected via biopsy.
During a conventional diagnostic procedure, surgery known as mediastinoscopy is performed to provide access to the chest. A small incision is made in the neck just above the breastbone or next to the breastbone. Next, a thin scope, called a mediastinoscope, is inserted through the opening to provide access to the lungs and surrounding lymph nodes. Tissue or fluid is then collected via biopsy.
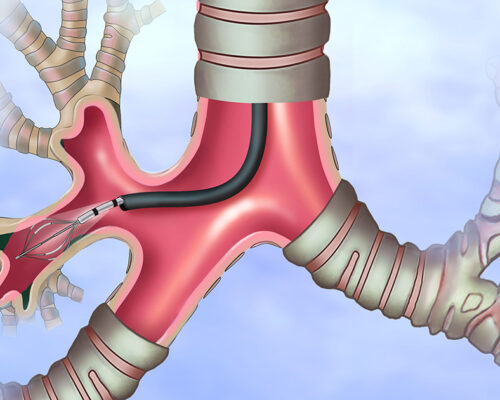
An endobronchial ultrasound is much less invasive.
- The physician can perform needle aspiration on lymph nodes using a bronchoscope inserted through the mouth
- A special endoscope fitted with an ultrasound processor and a fine-gauge aspiration needle is guided through the patient’s trachea
- No incisions are necessary
What are the Benefits of EBUS?

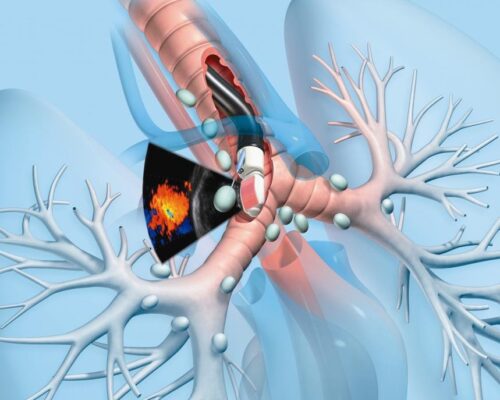
- It provides real-time imaging of the surface of the airways, blood vessels, lungs, and lymph nodes
- The improved images allow the physician to easily view difficult-to-reach areas and to access more, and smaller, lymph nodes for biopsy with the aspiration needle than through conventional mediatinoscopy
- The accuracy and speed of the EBUS procedure lends itself to rapid onsite pathologic evaluation Pathologists in the operating room can process and examine biopsy samples as they are obtained and can request additional samples to be taken immediately if needed
- EBUS is performed under moderate sedation or general anesthesia
- Patients recover quickly and can usually go home the same day
FAQs
What are the facilities available at the clinic?
The following facilities are available:
- Pulmonary function testing (Spirometry)
- Bronchoscopy
- EBUS
- Sleep studies (polysomnography)
- Thoracoscopy
- Lung cancer chemotherapy
I snore. Do I need to undergo a sleep study test?
It is not necessary that all persons who snore need to undergo a sleep study. There should be associated features to label it a disease. You should seek consultation from a sleep specialist in this case, who will screen you appropriately.
What will happen to my body if I sleep less?
Sleep is one of the key factors that determine the health of an individual. How one wakes up in the morning is a fair indicator whether one is getting a proper sleep or not. Therefore, if you have been snoozing your alarm too often, you might be damaging your own health. Experts believe that under normal circumstances, one should be able to wake up refreshed. And if you are not then you might be suffering from a sleep disorder. This can cause neurological changes in your body and can reduce the productivity at work. Moreover, in the short run it can cause memory problems and severe hormonal changes in your body.
Whatv is Pulmonary sleep test?
PFT measures how much air you can breathe in and out and how fast you can do it and how well your lungs are working to deliver oxygen to your blood. PFT is a painless test and a technician will ask you to take a deep breath and then blow as hard as you can into a tube connected to PFT machine.
PFT is the most important test for the diagnosis and management of COPD. PFT is similar to ECG of the lungs